Related Research Articles
An antianginal is a drug used in the treatment of angina pectoris, a symptom of ischaemic heart disease.

Coronary artery disease (CAD), also called coronary heart disease (CHD), ischemic heart disease (IHD), myocardial ischemia, or simply heart disease, involves the reduction of blood flow to the cardiac muscle due to build-up of atherosclerotic plaque in the arteries of the heart. It is the most common of the cardiovascular diseases. Types include stable angina, unstable angina, and myocardial infarction.

Angina, also known as angina pectoris, is chest pain or pressure, usually caused by insufficient blood flow to the heart muscle (myocardium). It is most commonly a symptom of coronary artery disease.
Microvascular angina (MVA), previously known as cardiac syndrome X, also known as coronary microvascular dysfunction(CMD) or microvascular coronary disease is a type of angina (chest pain) with signs associated with decreased blood flow to heart tissue but with normal coronary arteries.
Vasospasm refers to a condition in which an arterial spasm leads to vasoconstriction. This can lead to tissue ischemia and tissue death (necrosis). Cerebral vasospasm may arise in the context of subarachnoid hemorrhage. Symptomatic vasospasm or delayed cerebral ischemia is a major contributor to post-operative stroke and death especially after aneurysmal subarachnoid hemorrhage. Vasospasm typically appears 4 to 10 days after subarachnoid hemorrhage.

Acute coronary syndrome (ACS) is a syndrome due to decreased blood flow in the coronary arteries such that part of the heart muscle is unable to function properly or dies. The most common symptom is centrally located pressure-like chest pain, often radiating to the left shoulder or angle of the jaw, and associated with nausea and sweating. Many people with acute coronary syndromes present with symptoms other than chest pain, particularly women, older people, and people with diabetes mellitus.

Variant angina, also known as Prinzmetal angina,vasospastic angina, angina inversa, coronary vessel spasm, or coronary artery vasospasm, is a syndrome typically consisting of angina. Variant angina differs from stable angina in that it commonly occurs in individuals who are at rest or even asleep, whereas stable angina is generally triggered by exertion or intense exercise. Variant angina is caused by vasospasm, a narrowing of the coronary arteries due to contraction of the heart's smooth muscle tissue in the vessel walls. In comparison, stable angina is caused by the permanent occlusion of these vessels by atherosclerosis, which is the buildup of fatty plaque and hardening of the arteries.

Unstable angina is a type of angina pectoris that is irregular or more easily provoked. It is classified as a type of acute coronary syndrome.
Nitroglycerin, also known as glyceryl trinitrate (GTN), is a vasodilator used for heart failure, high blood pressure (hypertension), anal fissures, painful periods, and to treat and prevent chest pain caused by decreased blood flow to the heart (angina) or due to the recreational use of cocaine. This includes chest pain from a heart attack. It is taken by mouth, under the tongue, applied to the skin, or by injection into a vein.

Nicorandil is a vasodilator drug used to treat angina.
In medicine, collateralization, also vessel collateralization and blood vessel collateralization, is the growth of a blood vessel or several blood vessels that serve the same end organ or vascular bed as another blood vessel that cannot adequately supply that end organ or vascular bed sufficiently.
Myocardial stunning or transient post-ischemic myocardial dysfunction is a state of mechanical cardiac dysfunction that can occur in a portion of myocardium without necrosis after a brief interruption in perfusion, despite the timely restoration of normal coronary blood flow. In this situation, even after ischemia has been relieved and myocardial blood flow (MBF) returns to normal, myocardial function is still depressed for a variable period of time, usually days to weeks. This reversible reduction of function of heart contraction after reperfusion is not accounted for by tissue damage or reduced blood flow, but rather, its thought to represent a perfusion-contraction "mismatch". Myocardial stunning was first described in laboratory canine experiments in the 1970s where LV wall abnormalities were observed following coronary artery occlusion and subsequent reperfusion.
Abdominal angina is abdominal pain after eating that occurs in individuals with ongoing poor blood supply to their small intestines known as chronic mesenteric ischemia. Although the term angina alone usually denotes angina pectoris, angina by itself can also mean "any spasmodic, choking, or suffocative pain", with an anatomic adjective defining its focus; so, in this case, spasmodic pain in the abdomen. Stedman's Medical Dictionary Online defines abdominal angina as "intermittent abdominal pain, frequently occurring at a fixed time after eating, caused by inadequacy of the mesenteric circulation resulting from arteriosclerosis or other arterial disease. Synonym: intestinal angina."
Coronary artery anomalies are variations of the coronary circulation, affecting <1% of the general population. Symptoms include chest pain, shortness of breath and syncope, although cardiac arrest may be the first clinical presentation. Several varieties are identified, with a different potential to cause sudden cardiac death.

A nitrovasodilator is a pharmaceutical agent that causes vasodilation by donation of nitric oxide (NO), and is mostly used for the treatment and prevention of angina pectoris.

Coronary ischemia, myocardial ischemia, or cardiac ischemia, is a medical term for abnormally reduced blood flow in the coronary circulation through the coronary arteries. Coronary ischemia is linked to heart disease, and heart attacks. Coronary arteries deliver oxygen-rich blood to the heart muscle. Reduced blood flow to the heart associated with coronary ischemia can result in inadequate oxygen supply to the heart muscle. When oxygen supply to the heart is unable to keep up with oxygen demand from the muscle, the result is the characteristic symptoms of coronary ischemia, the most common of which is chest pain. Chest pain due to coronary ischemia commonly radiates to the arm or neck. Certain individuals such as women, diabetics, and the elderly may present with more varied symptoms. If blood flow through the coronary arteries is stopped completely, cardiac muscle cells may die, known as a myocardial infarction, or heart attack.
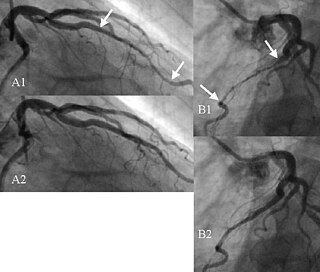
A myocardial bridge (MB) is a common congenital heart anomaly in which one of the coronary arteries tunnels through the heart muscle (myocardium) itself.
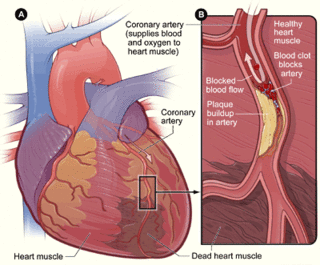
Management of acute coronary syndrome is targeted against the effects of reduced blood flow to the affected area of the heart muscle, usually because of a blood clot in one of the coronary arteries, the vessels that supply oxygenated blood to the myocardium. This is achieved with urgent hospitalization and medical therapy, including drugs that relieve chest pain and reduce the size of the infarct, and drugs that inhibit clot formation; for a subset of patients invasive measures are also employed. Basic principles of management are the same for all types of acute coronary syndrome. However, some important aspects of treatment depend on the presence or absence of elevation of the ST segment on the electrocardiogram, which classifies cases upon presentation to either ST segment elevation myocardial infarction (STEMI) or non-ST elevation acute coronary syndrome (NST-ACS); the latter includes unstable angina and non-ST elevation myocardial infarction (NSTEMI). Treatment is generally more aggressive for STEMI patients, and reperfusion therapy is more often reserved for them. Long-term therapy is necessary for prevention of recurrent events and complications.
Kounis syndrome is defined as acute coronary syndrome caused by an allergic reaction or a strong immune reaction to a drug or other substance. It is a rare syndrome with authentic cases reported in 130 males and 45 females, as reviewed in 2017; however, the disorder is suspected of being commonly overlooked and therefore much more prevalent. Mast cell activation and release of inflammatory cytokines as well as other inflammatory agents from the reaction leads to spasm of the arteries leading to the heart muscle or a plaque breaking free and blocking one or more of those arteries.
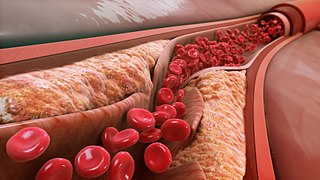
Arterial occlusion is a condition involving partial or complete blockage of blood flow through an artery. Arteries are blood vessels that carry oxygenated blood to body tissues. An occlusion of arteries disrupts oxygen and blood supply to tissues, leading to ischemia. Depending on the extent of ischemia, symptoms of arterial occlusion range from simple soreness and pain that can be relieved with rest, to a lack of sensation or paralysis that could require amputation.
References
- 1 2 3 4 5 6 7 8 Hung, Ming-Jui; Hu, Patrick; Hung, Ming-Yow (2014). "Coronary Artery Spasm: Review and Update". International Journal of Medical Sciences. 11 (11): 1161–1171. doi:10.7150/ijms.9623. ISSN 1449-1907. PMC 4166862 . PMID 25249785.
- 1 2 Prinzmetal, Myron; Kennamer, Rexford; Merliss, Reuben; Wada, Takashi; Bor, Naci (September 1959). "Angina pectoris I. A variant form of angina pectoris". The American Journal of Medicine. 27 (3): 375–388. doi:10.1016/0002-9343(59)90003-8. ISSN 0002-9343. PMID 14434946.
- 1 2 3 4 Cheng, Tsung O. (1972-05-01). "Variant Angina of Printzmetal with Normal Coronary Arteriograms: A Variant of the Variant". Annals of Internal Medicine. 76 (5): 862. doi:10.7326/0003-4819-76-5-862_2. ISSN 0003-4819.
- ↑ Robert, Chahine (1984). "Coronary Artery Spasm". JAMA: The Journal of the American Medical Association. 251 (8): 1097. doi:10.1001/JAMA.1984.03340320073040. S2CID 72379696.
- 1 2 3 Konst RE, Meeder JG, Wittekoek ME, Maas AH, Appelman Y, Piek JJ, et al. (August 2020). "Ischaemia with no obstructive coronary arteries". Netherlands Heart Journal. 28 (Suppl 1): 66–72. doi:10.1007/s12471-020-01451-9. PMC 7419395 . PMID 32780334.
- 1 2 3 4 Beltrame, John F.; Crea, Filippo; Kaski, Juan Carlos; Ogawa, Hisao; Ong, Peter; Sechtem, Udo; Shimokawa, Hiroaki; Bairey Merz, C. Noel; Group (COVADIS), On Behalf of the Coronary Vasomotion Disorders International Study (2017-09-01). "International standardization of diagnostic criteria for vasospastic angina". European Heart Journal. 38 (33): 2565–2568. doi: 10.1093/eurheartj/ehv351 . ISSN 0195-668X. PMID 26245334.
- 1 2 3 4 5 Yasue H, Nakagawa H, Itoh T, Harada E, Mizuno Y (February 2008). "Coronary artery spasm--clinical features, diagnosis, pathogenesis, and treatment". Journal of Cardiology. 51 (1): 2–17. doi: 10.1016/j.jjcc.2008.01.001 . PMID 18522770.
- 1 2 Yasue, Hirofumi; Kugiyama, Kiyotaka (1997). "Coronary Spasm: Clinical Features and Pathogenesis". Internal Medicine. 36 (11): 760–765. doi: 10.2169/internalmedicine.36.760 . ISSN 0918-2918. PMID 9392345.
- 1 2 3 4 5 6 Lanza GA, Careri G, Crea F (October 2011). "Mechanisms of coronary artery spasm". Circulation. 124 (16): 1774–82. doi: 10.1161/CIRCULATIONAHA.111.037283 . PMID 22007100.
- 1 2 Picard F, Sayah N, Spagnoli V, Adjedj J, Varenne O (January 2019). "Vasospastic angina: A literature review of current evidence". Archives of Cardiovascular Diseases. 112 (1): 44–55. doi: 10.1016/j.acvd.2018.08.002 . PMID 30197243.
- ↑ Talarico GP, Crosta ML, Giannico MB, Summaria F, Calò L, Patrizi R (May 2017). "Cocaine and coronary artery diseases: a systematic review of the literature". Journal of Cardiovascular Medicine. 18 (5): 291–294. doi:10.2459/JCM.0000000000000511. PMID 28306693. S2CID 13605509.
- 1 2 3 4 5 6 Matta A, Bouisset F, Lhermusier T, Campelo-Parada F, Elbaz M, Carrié D, Roncalli J (2020-05-15). "Coronary Artery Spasm: New Insights". Journal of Interventional Cardiology. 2020: 5894586. doi: 10.1155/2020/5894586 . PMC 7245659 . PMID 32508542.
- ↑ Jcs Joint Working Group (August 2010). "Guidelines for diagnosis and treatment of patients with vasospastic angina (coronary spastic angina) (JCS 2008): digest version". Circulation Journal. 74 (8): 1745–62. doi: 10.1253/circj.CJ-10-74-0802 . PMID 20671373.
- ↑ Matta, Anthony; Bouisset, Frederic; Lhermusier, Thibault; Campelo-Parada, Fran; Elbaz, Meyer; Carrié, Didier; Roncalli, Jerome (2020-05-15). "Coronary Artery Spasm: New Insights". Journal of Interventional Cardiology. 2020: 1–10. doi: 10.1155/2020/5894586 . PMC 7245659 . PMID 32508542.
- ↑ Itoh, Teruhiko; Mizuno, Yuji; Harada, Eisaku; Yoshimura, Michihiro; Ogawa, Hisao; Yasue, Hirofumi (2007). "Coronary Spasm is Associated With Chronic Low-Grade Inflammation". Circulation Journal. 71 (7): 1074–1078. doi: 10.1253/circj.71.1074 . ISSN 1346-9843. PMID 17587713.
- ↑ Messner Barbara; Bernhard David (2014-03-01). "Smoking and Cardiovascular Disease". Arteriosclerosis, Thrombosis, and Vascular Biology. 34 (3): 509–515. doi: 10.1161/ATVBAHA.113.300156 . PMID 24554606.
- ↑ Kusama, Yoshiki; Kodani, Eitaro; Nakagomi, Akihiro; Otsuka, Toshiaki; Atarashi, Hirotsugu; Kishida, Hiroshi; Mizuno, Kyoichi (2011). "Variant Angina and Coronary Artery Spasm: The Clinical Spectrum, Pathophysiology, and Management". Journal of Nippon Medical School. 78 (1): 4–12. doi: 10.1272/jnms.78.4 . ISSN 1347-3409. PMID 21389642.
- ↑ Shimokawa, Hiroaki (2000). "Cellular and Molecular Mechanisms of Coronary Artery Spasm". Japanese Circulation Journal. 64 (1): 1–12. doi: 10.1253/jcj.64.1 . ISSN 0047-1828. PMID 10651199.
- 1 2 3 Specchia, G.; de Servi, S. (1984), "Provocative Testing for Coronary Spasm", Breakdown in Human Adaptation to ‘Stress’, Dordrecht: Springer Netherlands, pp. 916–922, doi:10.1007/978-94-011-8064-1_70, ISBN 978-94-011-8066-5 , retrieved 2020-11-22
- 1 2 3 4 5 Slavich, Massimo; Patel, Riyaz Suleman (March 2016). "Coronary artery spasm: Current knowledge and residual uncertainties". IJC Heart & Vasculature. 10: 47–53. doi: 10.1016/j.ijcha.2016.01.003 . ISSN 2352-9067. PMC 5462634 . PMID 28616515.
- ↑ Robert, Chahine (1986). "Coronary Artery Spasm". Postgraduate Medicine. 79 (4): 78–91. doi:10.1080/00325481.1986.11699314.
- ↑ Robert A., Chahine (1983). Corronary Artery Spasm. Futura Publishing Company. ISBN 9780879931926.