
Vaccination is the administration of a vaccine to help the immune system develop immunity from a disease. Vaccines contain a microorganism or virus in a weakened, live or killed state, or proteins or toxins from the organism. In stimulating the body's adaptive immunity, they help prevent sickness from an infectious disease. When a sufficiently large percentage of a population has been vaccinated, herd immunity results. Herd immunity protects those who may be immunocompromised and cannot get a vaccine because even a weakened version would harm them. The effectiveness of vaccination has been widely studied and verified. Vaccination is the most effective method of preventing infectious diseases; widespread immunity due to vaccination is largely responsible for the worldwide eradication of smallpox and the elimination of diseases such as polio and tetanus from much of the world. However, some diseases, such as measles outbreaks in America, have seen rising cases due to relatively low vaccination rates in the 2010s – attributed, in part, to vaccine hesitancy. According to the World Health Organization, vaccination prevents 3.5–5 million deaths per year.

A vaccine is a biological preparation that provides active acquired immunity to a particular infectious or malignant disease. The safety and effectiveness of vaccines has been widely studied and verified. A vaccine typically contains an agent that resembles a disease-causing microorganism and is often made from weakened or killed forms of the microbe, its toxins, or one of its surface proteins. The agent stimulates the body's immune system to recognize the agent as a threat, destroy it, and recognize further and destroy any of the microorganisms associated with that agent that it may encounter in the future.
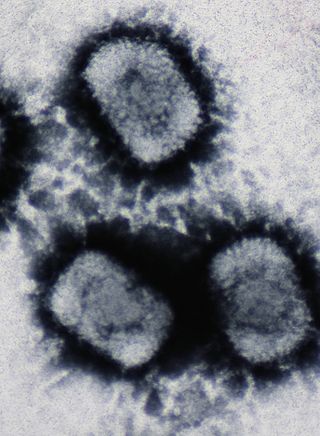
Cowpox is an infectious disease caused by the cowpox virus (CPXV). It presents with large blisters in the skin, a fever and swollen glands, historically typically following contact with an infected cow, though in the last several decades more often from infected cats. The hands and face are most frequently affected and the spots are generally very painful.

The smallpox vaccine is the first vaccine to have been developed against a contagious disease. In 1796, British physician Edward Jenner demonstrated that an infection with the relatively mild cowpox virus conferred immunity against the deadly smallpox virus. Cowpox served as a natural vaccine until the modern smallpox vaccine emerged in the 20th century. From 1958 to 1977, the World Health Organization (WHO) conducted a global vaccination campaign that eradicated smallpox, making it the only human disease to be eradicated. Although routine smallpox vaccination is no longer performed on the general public, the vaccine is still being produced to guard against bioterrorism, biological warfare, and mpox.
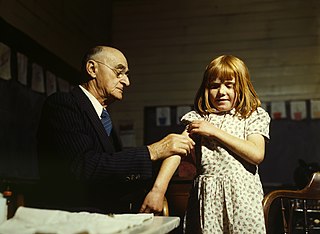
Immunization, or immunisation, is the process by which an individual's immune system becomes fortified against an infectious agent.
In biology, immunity is the state of being insusceptible or resistant to a noxious agent or process, especially a pathogen or infectious disease. Immunity may occur naturally or be produced by prior exposure or immunization.
This is a timeline of the development of prophylactic human vaccines. Early vaccines may be listed by the first year of development or testing, but later entries usually show the year the vaccine finished trials and became available on the market. Although vaccines exist for the diseases listed below, only smallpox has been eliminated worldwide. The other vaccine-preventable illnesses continue to cause millions of deaths each year. Currently, polio and measles are the targets of active worldwide eradication campaigns.

An exotoxin is a toxin secreted by bacteria. An exotoxin can cause damage to the host by destroying cells or disrupting normal cellular metabolism. They are highly potent and can cause major damage to the host. Exotoxins may be secreted, or, similar to endotoxins, may be released during lysis of the cell. Gram negative pathogens may secrete outer membrane vesicles containing lipopolysaccharide endotoxin and some virulence proteins in the bounding membrane along with some other toxins as intra-vesicular contents, thus adding a previously unforeseen dimension to the well-known eukaryote process of membrane vesicle trafficking, which is quite active at the host–pathogen interface.
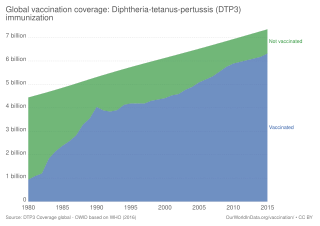
The DPT vaccine or DTP vaccine is a class of combination vaccines against three infectious diseases in humans: diphtheria, pertussis, and tetanus. The vaccine components include diphtheria and tetanus toxoids and either killed whole cells of the bacterium that causes pertussis or pertussis antigens. The term toxoid refers to vaccines which use an inactivated toxin produced by the pathogen which they are targeted against to generate an immune response. In this way, the toxoid vaccine generates an immune response which is targeted against the toxin which is produced by the pathogen and causes disease, rather than a vaccine which is targeted against the pathogen itself. The whole cells or antigens will be depicted as either "DTwP" or "DTaP", where the lower-case "w" indicates whole-cell inactivated pertussis and the lower-case "a" stands for "acellular". In comparison to alternative vaccine types, such as live attenuated vaccines, the DTP vaccine does not contain any live pathogen, but rather uses inactivated toxoid to generate an immune response; therefore, there is not a risk of use in populations that are immune compromised since there is not any known risk of causing the disease itself. As a result, the DTP vaccine is considered a safe vaccine to use in anyone and it generates a much more targeted immune response specific for the pathogen of interest.

A conjugate vaccine is a type of subunit vaccine which combines a weak antigen with a strong antigen as a carrier so that the immune system has a stronger response to the weak antigen.

A toxoid is an inactivated toxin whose toxicity has been suppressed either by chemical (formalin) or heat treatment, while other properties, typically immunogenicity, are maintained. Toxins are secreted by bacteria, whereas toxoids are altered form of toxins; toxoids are not secreted by bacteria. Thus, when used during vaccination, an immune response is mounted and immunological memory is formed against the molecular markers of the toxoid without resulting in toxin-induced illness. Such a preparation is also known as an anatoxin. There are toxoids for prevention of diphtheria, tetanus and botulism.
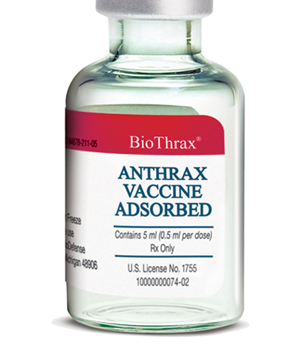
Anthrax vaccines are vaccines to prevent the livestock and human disease anthrax, caused by the bacterium Bacillus anthracis.
The following are notable events in the Timeline of immunology:
In immunology, passive immunity is the transfer of active humoral immunity of ready-made antibodies. Passive immunity can occur naturally, when maternal antibodies are transferred to the fetus through the placenta, and it can also be induced artificially, when high levels of antibodies specific to a pathogen or toxin are transferred to non-immune persons through blood products that contain antibodies, such as in immunoglobulin therapy or antiserum therapy. Passive immunization is used when there is a high risk of infection and insufficient time for the body to develop its own immune response, or to reduce the symptoms of ongoing or immunosuppressive diseases. Passive immunization can be provided when people cannot synthesize antibodies, and when they have been exposed to a disease that they do not have immunity against.
Immunization during pregnancy is the administration of a vaccine to a pregnant individual. This may be done either to protect the individual from disease or to induce an antibody response, such that the antibodies cross the placenta and provide passive immunity to the infant after birth. In many countries, including the US, Canada, UK, Australia and New Zealand, vaccination against influenza, COVID-19 and whooping cough is routinely offered during pregnancy.

Hepatitis B vaccine is a vaccine that prevents hepatitis B. The first dose is recommended within 24 hours of birth with either two or three more doses given after that. This includes those with poor immune function such as from HIV/AIDS and those born premature. It is also recommended that health-care workers be vaccinated. In healthy people, routine immunization results in more than 95% of people being protected.

Pertussis vaccine is a vaccine that protects against whooping cough (pertussis). There are two main types: whole-cell vaccines and acellular vaccines. The whole-cell vaccine is about 78% effective while the acellular vaccine is 71–85% effective. The effectiveness of the vaccines appears to decrease by between 2 and 10% per year after vaccination with a more rapid decrease with the acellular vaccines. The vaccine is only available in combination with tetanus and diphtheria vaccines. Pertussis vaccine is estimated to have saved over 500,000 lives in 2002.
Variolation was the method of inoculation first used to immunize individuals against smallpox (Variola) with material taken from a patient or a recently variolated individual, in the hope that a mild, but protective, infection would result. Only 1–2% of those variolated died from the intentional infection compared to 30% who contracted smallpox naturally. Variolation is no longer used today. It was replaced by the smallpox vaccine, a safer alternative. This in turn led to the development of the many vaccines now available against other diseases.
Inoculation is the act of implanting a pathogen or other microbe or virus into a person or other organism. It is a method of artificially inducing immunity against various infectious diseases. The term "inoculation" is also used more generally to refer to intentionally depositing microbes into any growth medium, as into a Petri dish used to culture the microbe, or into food ingredients for making cultured foods such as yoghurt and fermented beverages such as beer and wine. This article is primarily about the use of inoculation for producing immunity against infection. Inoculation has been used to eradicate smallpox and to markedly reduce other infectious diseases such as polio. Although the terms "inoculation", "vaccination", and "immunization" are often used interchangeably, there are important differences. Inoculation is the act of implanting a pathogen or microbe into a person or other recipient; vaccination is the act of implanting or giving someone a vaccine specifically; and immunization is the development of disease resistance that results from the immune system's response to a vaccine or natural infection.

Animal vaccination is the immunisation of a domestic, livestock or wild animal. The practice is connected to veterinary medicine. The first animal vaccine invented was for chicken cholera in 1879 by Louis Pasteur. The production of such vaccines encounter issues in relation to the economic difficulties of individuals, the government and companies. Regulation of animal vaccinations is less compared to the regulations of human vaccinations. Vaccines are categorised into conventional and next generation vaccines. Animal vaccines have been found to be the most cost effective and sustainable methods of controlling infectious veterinary diseases. In 2017, the veterinary vaccine industry was valued at US$7 billion and it is predicted to reach US$9 billion in 2024.












