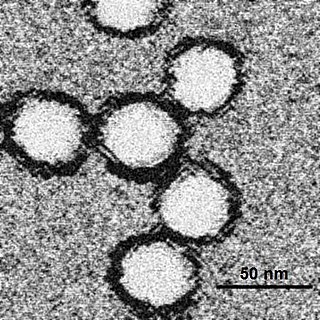
West Nile fever is an infection by the West Nile virus, which is typically spread by mosquitoes. In about 80% of infections people have few or no symptoms. About 20% of people develop a fever, headache, vomiting, or a rash. In less than 1% of people, encephalitis or meningitis occurs, with associated neck stiffness, confusion, or seizures. Recovery may take weeks to months. The risk of death among those in whom the nervous system is affected is about 10 percent.
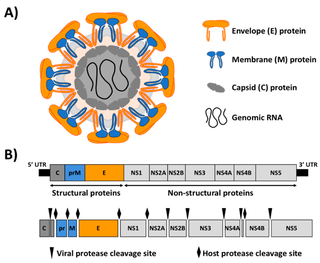
Flaviviridae is a family of enveloped positive-strand RNA viruses which mainly infect mammals and birds. They are primarily spread through arthropod vectors. The family gets its name from the yellow fever virus; flavus is Latin for "yellow", and yellow fever in turn was named because of its propensity to cause jaundice in victims. There are 89 species in the family divided among four genera. Diseases associated with the group include: hepatitis (hepaciviruses), hemorrhagic syndromes, fatal mucosal disease (pestiviruses), hemorrhagic fever, encephalitis, and the birth defect microcephaly (flaviviruses).
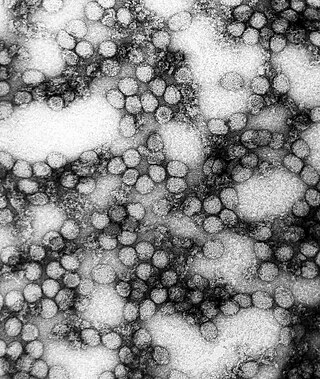
Flavivirus, renamed Orthoflavivirus in 2023, is a genus of positive-strand RNA viruses in the family Flaviviridae. The genus includes the West Nile virus, dengue virus, tick-borne encephalitis virus, yellow fever virus, Zika virus and several other viruses which may cause encephalitis, as well as insect-specific flaviviruses (ISFs) such as cell fusing agent virus (CFAV), Palm Creek virus (PCV), and Parramatta River virus (PaRV). While dual-host flaviviruses can infect vertebrates as well as arthropods, insect-specific flaviviruses are restricted to their competent arthropods. The means by which flaviviruses establish persistent infection in their competent vectors and cause disease in humans depends upon several virus-host interactions, including the intricate interplay between flavivirus-encoded immune antagonists and the host antiviral innate immune effector molecules.

Japanese encephalitis (JE) is an infection of the brain caused by the Japanese encephalitis virus (JEV). While most infections result in little or no symptoms, occasional inflammation of the brain occurs. In these cases, symptoms may include headache, vomiting, fever, confusion and seizures. This occurs about 5 to 15 days after infection.
Murray Valley encephalitis virus (MVEV) is a zoonotic flavivirus endemic to northern Australia and Papua New Guinea. It is the causal agent of Murray Valley encephalitis. In humans, it can cause permanent neurological disease or death. MVEV is related to Kunjin virus, which has a similar ecology, but a lower morbidity rate. Although the arbovirus is endemic to Northern Australia, it has occasionally spread to the southern states during times of heavy rainfall during the summer monsoon season via seasonal flooding of the Murray-Darling River system. These outbreaks can be "...decades apart, with no or very few cases identified in between".

Alphavirus is a genus of RNA viruses, the sole genus in the Togaviridae family. Alphaviruses belong to group IV of the Baltimore classification of viruses, with a positive-sense, single-stranded RNA genome. There are 32 alphavirus species, which infect various vertebrates such as humans, rodents, fish, birds, and larger mammals such as horses, as well as invertebrates. Alphaviruses that can infect both vertebrates and arthropods are referred dual-host alphaviruses, while insect-specific alphaviruses such as Eilat virus and Yada yada virus are restricted to their competent arthropod vector. Transmission between species and their vertebrate hosts occurs mainly via mosquitoes, making the alphaviruses a member of the collection of arboviruses – or arthropod-borne viruses. Alphavirus particles are enveloped, have a 70 nm diameter, tend to be spherical, and have a 40 nm isometric nucleocapsid.

Thogotovirus is a genus of enveloped RNA viruses, one of seven genera in the virus family Orthomyxoviridae. Their single-stranded, negative-sense RNA genome has six or seven segments. Thogotoviruses are distinguished from most other orthomyxoviruses by being arboviruses – viruses that are transmitted by arthropods, in this case usually ticks. Thogotoviruses can replicate in both tick cells and vertebrate cells; one subtype has also been isolated from mosquitoes. A consequence of being transmitted by blood-sucking vectors is that the virus must spread systemically in the vertebrate host – unlike influenza viruses, which are transmitted by respiratory droplets and are usually confined to the respiratory system.

Venezuelan equine encephalitis virus is a mosquito-borne viral pathogen that causes Venezuelan equine encephalitis or encephalomyelitis (VEE). VEE can affect all equine species, such as horses, donkeys, and zebras. After infection, equines may suddenly die or show progressive central nervous system disorders. Humans also can contract this disease. Healthy adults who become infected by the virus may experience flu-like symptoms, such as high fevers and headaches. People with weakened immune systems and the young and the elderly can become severely ill or die from this disease.
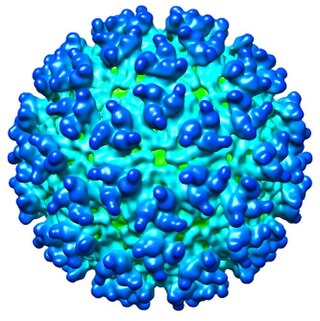
The Western equine encephalomyelitis virus is the causative agent of relatively uncommon viral disease Western equine encephalomyelitis (WEE). An alphavirus of the family Togaviridae, the WEE virus is an arbovirus transmitted by mosquitoes of the genera Culex and Culiseta. WEE is a recombinant virus between two other alphaviruses, an ancestral Sindbis virus-like virus, and an ancestral Eastern equine encephalitis virus-like virus. There have been under 700 confirmed cases in the U.S. since 1964. This virus contains an envelope that is made up of glycoproteins and nucleic acids. The virus is transmitted to people and horses by bites from infected mosquitoes and birds during wet, summer months.

B-virus, Herpesvirus simiae, or Herpes virus B is the Simplexvirus infecting macaque monkeys. B virus is very similar to HSV-1, and as such, this neurotropic virus is not found in the blood.
Visna-maedi virus from the genus Lentivirus and subfamily Orthoretrovirinae, is a retrovirus that causes encephalitis and chronic pneumonitis in sheep. It is known as visna when found in the brain, and maedi when infecting the lungs. Lifelong, persistent infections in sheep occur in the lungs, lymph nodes, spleen, joints, central nervous system, and mammary glands; The condition is sometimes known as ovine progressive pneumonia (OPP), particularly in the United States, or Montana sheep disease. White blood cells of the monocyte/macrophage lineage are the main target of the virus.

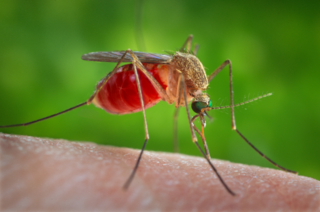
Mosquito-borne diseases or mosquito-borne illnesses are diseases caused by bacteria, viruses or parasites transmitted by mosquitoes. Nearly 700 million people contract mosquito-borne illnesses each year, resulting in more than a million deaths.
Rocio viral encephalitis is an epidemic flaviviral disease of humans first observed in São Paulo State, Brazil, in 1975. Low-level enzootic transmission is likely continuing in the epidemic zone, and with increased deforestation and population expansion, additional epidemics caused by Rocio virus are highly probable. If migratory species of birds are, or become involved in, the virus transmission cycle, the competency of a wide variety of mosquito species for transmitting Rocio virus experimentally suggest that the virus may become more widely distributed. The encephalitis outbreak in the western hemisphere caused by West Nile virus, a related flavivirus, highlights the potential for arboviruses to cause severe problems far from their source enzootic foci.
Culex quinquefasciatus, commonly known as the southern house mosquito, is a medium-sized mosquito found in tropical and subtropical regions of the world. It is a vector of Wuchereria bancrofti, avian malaria, and arboviruses including St. Louis encephalitis virus, Western equine encephalitis virus, Zika virus and West Nile virus. It is taxonomically regarded as a member of the Culex pipiens species complex. Its genome was sequenced in 2010, and was shown to have 18,883 protein-coding genes.
Jamestown Canyon encephalitis is an infectious disease caused by the Jamestown Canyon virus, an orthobunyavirus of the California serogroup. It is mainly spread during the summer by different mosquito species in the United States and Canada.
Spondweni virus is an arbovirus, or arthropod-borne virus, which is a member of the family Flaviviridae and the genus Flavivirus. It is part of the Spondweni serogroup which consists of the Sponweni virus and the Zika virus (ZIKV). The Spondweni virus was first isolated in Nigeria in 1952, and ever since, SPONV transmission and activity have been reported throughout Africa. Its primary vector of transmission is the sylvatic mosquito Aedes circumluteolus, though it has been isolated from several different types of mosquito. Transmission of the virus into humans can lead to a viral infection known as Spondweni fever, with symptoms that include headache, nausea, myalgia and arthralgia. However, as SPONV is phylogenetically close to the ZIKV, it is commonly misdiagnosed as ZIKV along with other viral illnesses.

West Nile virus (WNV) is a single-stranded RNA virus that causes West Nile fever. It is a member of the family Flaviviridae, from the genus Flavivirus, which also contains the Zika virus, dengue virus, and yellow fever virus. The virus is primarily transmitted by mosquitoes, mostly species of Culex. The primary hosts of WNV are birds, so that the virus remains within a "bird–mosquito–bird" transmission cycle. The virus is genetically related to the Japanese encephalitis family of viruses. Humans and horses both exhibit disease symptoms from the virus, and symptoms rarely occur in other animals.

Culex nigripalpus is a species of medium-sized, dark, blood-feeding mosquito of the family Culicidae.
Yokose virus (YOKV) is in the genus Flavivirus of the family Flaviviridae. Flaviviridae are often found in arthropods, such as mosquitoes and ticks, and may also infect humans. The genus Flavivirus includes over 50 known viruses, including Yellow Fever, West Nile Virus, Zika Virus, and Japanese Encephalitis. Yokose virus is a new member of the Flavivirus family that has only been identified in a few bat species. Bats have been associated with several emerging zoonotic diseases such as Ebola and SARS.

Portogloboviridae is a family of dsDNA viruses that infect archaea. It is a proposed family of the realm Varidnaviria, but ICTV officially puts it as incertae sedis virus. Viruses in the family are related to Helvetiavirae. The capsid proteins of these viruses and their characteristics are of evolutionary importance for the origin of the other Varidnaviria viruses since they seem to retain primordial characters.















